Supporting local independent businesses has always been promoted here. Our local businesses keep money flowing within our community instead of transferring it out of town, or even out of state. And yet, when it comes to healthcare, keeping things local is harder than ever.
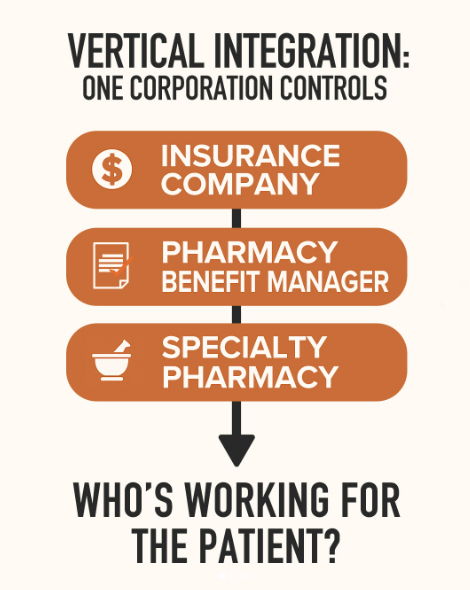
At present, three major companies control an essential part of our healthcare system. A vertically integrated strategy that combines pharmaceutical manufacturers, health benefit managers, insurance companies and chain pharmacies is gaming the system and driving independent pharmacies out of business. Last year, roughly 300 independent pharmacies closed up shop across America.
The lynchpin holding the scheme together is the dominance of three pharmacy benefit manager companies, the entities that act as middlemen between the other players. Pharmacy benefit managers establish the formularies that insurance companies can offer policy holders. Formularies are the list of pharmaceuticals that an insurance carrier will pay for. If a prescription drug is not on the formulary list, patients are out of luck and must pay out-of-pocket costs, often extraordinarily high.
Vertical integration means that a pharmacy benefit manager not only negotiates with pharmaceutical companies competing to be included on a formulary, but also sets the purchase price paid by each pharmacy and ultimately the amount that an insurance company will pay the pharmacy when it fills a prescription. In other words, business transactions that normally would be considered to be conflicts of interest are now everyday activities.
A prime example of vertical integration is CVS, a national chain of pharmacies which combines insurance (Aetna), pharmacy benefit management (Caremark), retail pharmacies, and clinical care (Oak Street Health) into a single entity to control costs and patient care. As pharmacy benefit manager, the company steers consumers to their 9,000 affiliated pharmacies, effectively cutting out independents.
Moreover, the control of reimbursement rates creates economic hardship for independents. For example, Aman Garg, owner of our only independent local pharmacy, Adobe Drugs, explains that to fill a prescription minimally costs him about $12, which includes staff time, bottles, labels, and allocated overhead costs. If he carries a drug, he is required to fill a prescription for it, but the reimbursement rate set by the pharmacy benefit manager is sometimes as low as thirty-five cents. In other words, he loses money. His only choice is to not carry the drug at all, which then deprives the consumer of obtaining what they need. It’s crazy.
This problem built slowly. Pharmacy benefit managers were created to provide businesses and insurance companies an efficient way to manage the millions of prescriptions generated each year, but they have become the tail wagging the healthcare dog. Their power is now so great that they effectively create what used to be called anti-trust activities and promote a trend towards monopoly. For the independent pharmacies, it’s a death sentence.
It’s not within the power of the local government to solve this problem, but the state government can. As the cost of healthcare increases steadily, legislation is needed to eliminate the self-dealing that is now commonplace. We call upon our elected representatives in Sacramento to enact regulations that bring these unethical practices to a halt and restore equity to this segment of healthcare. It’s either that, or we can kiss our locally owned and operated pharmacy goodbye.









Be First to Comment